Common Paediatric ENT conditions
There are a number of common ENT conditions that affect paediatric patients including:
- Recurrent nose bleeds (Epstaxis)
- Recurrent tonsilitis
- Snoring / Obstructive sleep apnea
- Hearing issues
Dr Crawford has extensive experience in the diagnosis, treatment and management of paediatric ENT patients over the age of 12 months.
Paediatric Nose Bleeds (Epistaxis)
Episodes of nose bleeds (Epistaxis) are common in children and are often spontaneous and stop without treatment. Nose bleeds are the result of small blood vessels inside the nose bursting. This most commonly occurs from the septum which divides the nose into two cavities and is often caused by minor trauma such as nose picking, rubbing, sneezing, coughing, or straining. In normal circumstances, the bleed will resolve quickly on its own as the blood clots and forms a scab, and the vessel then heals.
When to seek treatment for epistaxis?
If your child is under two years of age or has nose bleeds that happen frequently (more than 2- 3 times per month), looks pale or anaemic, or has bleeding that does not stop on its own after 10 minutes, they should be seen by your General Practitioner (GP) for assessment and determination of referral to a paediatric ENT Specialist.
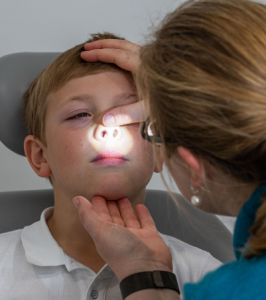
How is epistaxis treated?
In the first instance, Dr Crawford will conduct an examination to properly diagnose epistaxis. To do this, she uses a tiny camera to look inside the nose and throat of your child. This provides her with a magnified view and helps identify the difference between allergy symptoms, infection, and structural or developmental causes. When a vessel in the nose is identified as the source of bleeding, the most common treatment is cauterisation to create an area of toughened tissue to prevent further bleeding.
During the diagnosis examination if Dr Crawford determines it suitable, complete cauterisation can also be performed with minimal side effects.
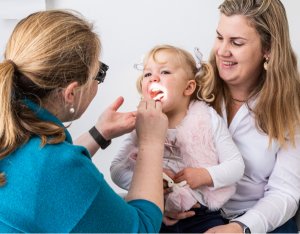
Tonsilitis
Tonsillitis is a common infection in children usually caused by viruses, but it can sometimes be the result of a bacterial infection – most commonly from strep bacteria. Symptoms for tonsillitis include:
- A very sore throat
- Scratchy sounding voice
- Bad breath
- Fever
- Ear ache
- Stomach ache
- Stiff neck
Tonsillitis is generally not a cause for concern unless the condition occurs repeatedly.
Diagnosis of tonsilitis
If your child is suffering from any of the listed symptoms, your GP will be able to determine whether it is tonsilitis from a physical examination that involves feeling the sides of the neck to check for swelling and pain, and checking if the tonsils are red or swollen, or if they have pus on them. Your GP should also check for fever, and examine your child’s ears and nose for signs of infection.
If it is determined that your child suffers from tonsillitis, and then has multiple illnesses of tonsilitis in a short time, you should ask your General Practitioner to organise a referral to a paediatric ENT specialist.
How is tonsilitis treated?
If your child is suffering from strep throat it can often be effectively managed with antibiotics. However, if you child has recurrent tonsilitis it may be necessary to remove their tonsils.
Dr Crawford treats children with recurrent tonsilitis and will be able to discuss with you the different management and treatment options for your child’s continued good health and well-being. At your consultation, she will examine your child and provide advice on the best management and treatment options and advise whether a tonsillectomy (the surgical removal of the tonsils) is recommended. Please call us today to arrange for an appointment at our rooms in Hurstville or Darlinghurst.
Snoring and Obstructive Sleep Apnea (OSA) in children
In children, Obstructive Sleep Apnea (OSA) is often a result of enlarged tonsils or adenoids. Parents often report symptoms of snoring, noisy breathing, pauses in breathing during sleep, and a restless sleeper. Younger children cannot always describe what is happening or what sensation or part of their body is causing pain or discomfort.
Often times these symptoms are mild and will be outgrown by children. However, if your child has OSA it can result in a failure to thrive and lead to ongoing medical conditions.
If you child has persistent OSA symptoms, it is important to have them assessed to ensure their ongoing health, well-being, and development is not impacted. When you attend your GP, you should discuss your concerns and they will provide a referral to a paediatric ENT specialist for further assessment.
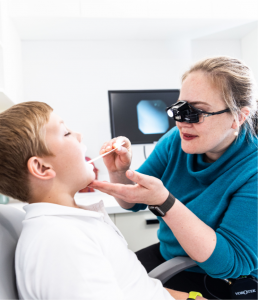
How is OSA in children diagnosed?
When assessing your child for sleep apnea, Dr Julia Crawford often uses a tiny camera to look inside their nose and throat . Having a magnified view helps her identify the difference between allergy symptoms, infection, and structural or developmental causes.
After the examination, she may then refer your child for more testing and investigation (such as allergy testing or a Sleep Study) before making a diagnosis. Based on these results and the information provided from parents and caregivers, Dr Crawford can better understand the child and advise what treatments are best suited to improve their condition.
How is OSA in children treated?
There are multiple non-surgical management and treatment options that Dr Crawford can provide including lifestyle management for obese children, to surgery for the removal of enlarged tonsils and adenoids. Each child is different, and the treatment and management recommended depends upon the cause of the condition.
If your child has symptoms of sleep apnea, please arrange for a referral from your GP and call our team to arrange for an appointment.

Signs of hearing issues causing speech delay in children
A child may be suspected of having a speech delay if a parent, career, babysitter, or preschool teacher notice any of the following:
- The child speaks fewer words than their age peers.
- They are less responsive to spoken instruction in a group setting.
- They are not easily understood by people outside the family unit.
If you believe your child has a speech delay, it is best to discuss this with your GP in the first instance to rule out other developmental delays. If no global developmental delay is suspected, you should request a referral for a hearing test and a consultation with a paediatric Ear, Nose, and Throat Specialist such as Dr Crawford.
Glue ear (OME)
A common cause for Speech Delay in children is Glue Ear, medically known as Otitis Media with Effusion or OME.
Glue Ear or OME is the build-up of fluid behind the eardrum and is diagnosed by a hearing test that shows interruption to hearing or conductive hearing loss.
If you child is referred to Dr Crawford with a suspicion of Glue Ear, to ensure a correct diagnosis and before embarking on treatment, she will recommend an initial and then a repeat hearing test after a period of monitoring.
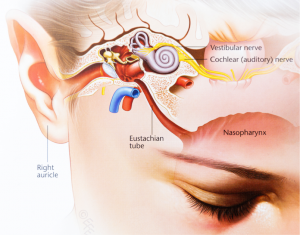
Treatment for Glue ear
If testing and monitoring shows there is no improvement in your child’s hearing, the gold standard treatment for glue ear involves a minor surgical procedure which involves the insertion of grommets. Grommets are tiny tubes inserted into your child’s eardrum that allow the fluid to drain away from the middle ear until the eustachean tubes mature to work naturally. This is a simple day surgery procedure performed under general anaesthetic and often children feel no pain afterwards. The grommets generally remain in place anywhere from 6-18 months and then fall out by themselves.
If your child has been diagnosed with glue ear or you are seeking to confirm a diagnosis and treatment, please call our team to arrange for a consultation with Dr Crawford. She will discuss with you any tests required and all aspects of the treatment involved.
Recommendation for paediatric ENT surgery
Each child is individual, and Dr Crawford ensures a complete investigation and diagnosis before recommending surgical treatment for paediatric ENT conditions.
If your child has an ENT condition that you are concerned about, please call and arrange for a consultation at our rooms in Darlinghurst or Kogarah.
