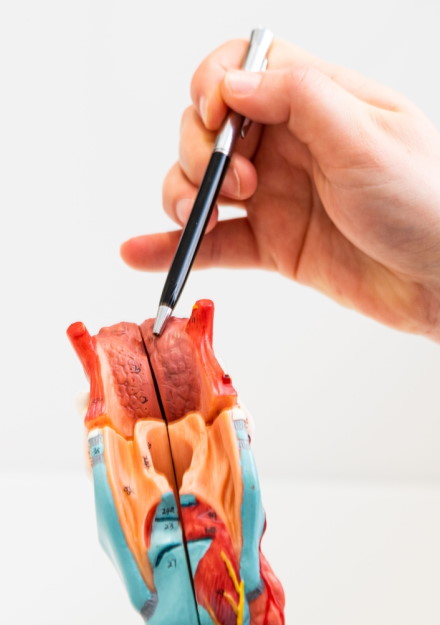
What is Obstructive Sleep Apnoea (OSA)?
Obstructive Sleep Apnoea is when there is a partial or complete blockage of the throat and airway, which causes a person to stop breathing in their sleep. Obstructive Sleep Apnoea in adults is often caused by a narrowing of the throat and face structures. OSA in adults may be accompanied by other health concerns such as high blood pressure, heart conditions, and obesity.
OSA is a common disorder that affects thousands of Australians. According to a study, about 4% of the total Australian population aged 20-65 years suffer from moderate to severe obstructive sleep apnoea.
The economic burden of OSA is staggering. Economic estimates reveal that healthcare costs due to OSA have already surpassed AU$13 billion annually. OSA is also a significant cause of decreased productivity, translating to AU$25 billion in lost GDP for the Australian economy.
OSA can have detrimental effects on sleep quality and health. It is associated with a diminished quality of life and serious medical comorbidities. OSA in adults may be accompanied by other health conditions such as high blood pressure, heart disease, type 2 diabetes, depression and obesity.
Men, especially older males, are usually prone to developing OSA and are considered a priority group for preventive interventions. Lifestyle interventions such as stopping smoking and alcohol consumption, weight loss, and increasing physical activity can help.
Reducing the occurrence of OSA by 10% would have a substantial impact on our healthcare system, preventing 16701 deaths, 47,542 cardiovascular events, 88,583 episodes of major depression and 476 vehicle-related accidents. Effective diagnosis and successful treatment of OSA can reduce symptoms and improve the quality of life of patients.
Dr Julia Crawford specialises in the surgical treatment of Obstructive Sleep Apnoea or OSA. She undertook a six-month subspecialty fellowship in surgery for OSA to learn about assessing and implementing treatment and care for people with OSA who meet the criteria for surgical intervention.
What are the symptoms of OSA?
Sleep related breathing disorders are marked by abnormal breathing or respiration during sleep. There are four major groups of sleep-related breathing disorders: obstructive sleep apnoea (OSA), central sleep apnoea, hypoventilation and hypoxemia. OSA is the most common out of these disorders.
Pauses in breathing caused by Obstructive Sleep Apnoea may vary between a few seconds, up to a minute or more. This is due to recurrent episodes or complete or partial closure of the upper airway. A person with Obstructive Sleep Apnoea may feel like their sleep quality is poor, that they snore loudly, toss, or turn a lot in their sleep, or frequently wake during the night. If you have OSA, you may wake tired and tire easily during the day. A bed partner or parent may also observe breathing pauses and report the severity of snoring and behaviour changes such as increased tiredness, irritability, and depression.
How is OSA diagnosed?
To have sleep apnoea diagnosed, you need first need to consult a sleep specialist/doctor. Your physician will check for signs and symptoms and a physical examination. If you are referred to an ENT surgeon for the initial assessment they will also examine your upper airway with a nasendoscopy/larnygosocpy to try and assess where your airway is collapsing. To confirm a diagnosis of OSA you will need to have a sleep study or polysomogram performed. It some instances, the ENT surgeon can refer you directly for this but often the referral, in order to be medicare rebate eligible, will need to come from a sleep physician/doctor.
An Obstructive Sleep Apnoea diagnosis is given after a Sleep Study is completed where sensors track sleep patterns, breathing, and oxygen levels. This can be done by either a formal Polysomogram in an overnight sleep study lab or as a Home Sleep Study. For a sleep study to be performed, patients need to be reviewed by a Respiratory Physician or Sleep doctor.
- In Lab Polysomnography (Level I Sleep Study). Under this laboratory sleep study, you will be hooked up to a device that monitors your heart, lung and brain activity, air pressure, breathing rhythm, movements, and blood oxygen levels while you sleep. Your sleep state will be monitored completely or partially through the night. The sleep study may also evaluate you for other sleep disorders that result in daytime sleepiness or require other kinds of treatment.
- Home sleep apnoea test (Level II Sleep Study). Another option is to do the polysomnography test at home, rather than at a sleep center. This involves the use of a simlar breathing monitor that tracks your breathing frequency, pattern and effort, as well as your oxygen levels. The downside is that it is sometimes not as comprehensive as an in lab sleep study but on the upside, it is performed in the comfort of your own bed
Obstructive Sleep Apnoea Treatment (Non-Surgical)
Once you have been diagnosed with OSA, there is a range of treatment options to consider. Dr Julia Crawford works through the most up to date and suitable options available in treating sleep apnoea, from non-invasive through to surgical options.
Every patient’s case is individual, and treatment options for sleep apnoea depends on what structures are most likely to be causing an obstruction during sleep such as nasal congestion. If examination shows that you may be best assisted with non-surgical treatment there are one of two devices that can help stabilise the body while sleeping to ensure waking up well-rested and ready for the day.
Mandibular Advancement Splint (MAS)
Dr Julia Crawford may recommend a Mandibular Advancement Splint (MAS) based on an examination of your airway. A Mandibular Advancement Split works like a mouthguard that you wear while you sleep. The MAS changes the position of your jaw while you are wearing it, bringing your chin forward, making more space in the back of your throat for your tongue. It can also help to stabilise the soft palate and uvula.
To have a MAS made, Dr Crawford may ask for your dentists details or refer you to a specialist dentist. A Mandibular Advancement Splint is not invasive and does not require any special care or treatment. Your self-evaluation of tiredness, surveys, and follow up testing such as a repeated Sleep Study will confirm if the MAS has improved your quality of sleep.
Continuous Positive Airway Pressure (CPAP)
In some instances, Dr Crawford may refer you to a specialist Respiratory Physician or Sleep Doctor or refer you back to your Sleep Doctor for a trial of a Continuous Positive Airway Pressure (CPAP) or CPAP machine. A CPAP device consists of a mask you wear over your nose and mouth while sleeping and a pump that delivers air.
CPAP works to make sure your airway always stays open by creating a flow of air into your nose or mouth to prevent structural collapse. The airflow created by CPAP machines is gentle and does not affect your ability to breathe normally. Continuous Positive Airway Pressure is a common and often successful non-surgical and minimally invasive treatment for sleep apnoea. Your self-evaluation of tiredness, surveys, and follow-up testing such as a repeated Sleep Study will confirm if CPAP has improved your sleep quality.
When is surgical treatment an option for Sleep Apnoea (OSA)?
Some people’s symptoms do not significantly improve with MAS or CPAP as they may have other structural causes of Obstructive Sleep Apnoea. In these cases, surgical intervention may be the best option. If you have utilised MAS or CPAP and have not achieved improved sleep quality, Dr Crawford can assess whether surgery is a suitable treatment option for you.
Below are the different surgical approaches that may be performed:
- Uvulopalatopharyngoplasty (UPPP) is a kind of surgery to open the upper airways by the removal of the tonsil tissueand a rearrangement of the soft palate.. It can be done as a solution for mild or moderate sleep apnoea.
- Hypoglossal Nerve Stimulator Implant. This device is an impulse generator that’s implanted under the skin of the upper chest. The device monitors a patient’s breathing patterns and stimulates the upper airway, specifically nerves that control tongue movement. This is currently not, as yet, available in Australia but hopefully will be by 2024.
- Maxillomandibular Advancement (MMA) Surgery. This procedure is effective for treating severe obstructive sleep apnoea. It involves the repositioning of the bones of the upper and lower jaw to alleviate airway obstruction. This creates a space behind the tongue and soft palate, preventing obstruction. If Dr Crawford thinks that you may benefit from this intervention, she will refer you on to a sleep trained oromaxillofacial surgeon
- Nasal Surgery. Nasal obstruction can make it more difficult for people to feel like they get a refreshing sleep and may make it more difficult to use devices like CPAP or MAS. Nasal surgery to alleviate nasal obstruction is unlikely to have any significant impact on the severity of OSA, however it can sometimes mean that patients will then be able to tolerate CPAP therapy better.
To arrange for a consultation, please arrange for a referral from your GP or Sleep Doctor and contact our team on 02 8319 9434.
FREQUENTLY ASKED QUESTIONS
Obstructive sleep apnoea happens when the muscles in the back of your throat collapse during sleep causing a drop in your oxygen blood levels which sends a message to your brain to pull you out of deep sleep into light sleep. In light sleep the muscles tense up again opening your airway. This cycle repeats throughout the night meaning that you never get restorative sleep.
Making lifestyle changes, such as maintaining a healthy weight (and shedding off excess weight), exercising regularly, drinking alcohol moderately, and quitting smoking can help prevent OSA. Sleep position also plays a factor, for some patients, sleeping on the side can stop the apnoea from occurring.
OSA happens when you can’t breathe normally due to upper airway obstruction. On the other hand, central sleep apnoea occurs when your brain doesn’t send proper signals to the muscles that are responsible for your breathing. Unfortunately, there are no surgical options to treat central OSA.
